Glioblastoma, a fast growing type of brain tumour that belongs to a group of gliomas, stands as one of the most aggressive and most challenging cancers the medicine has ever faced.
For decades, the medical community has tried hard to find effective ways to battle against this devastating disease.
While standard treatments such as surgery, chemotherapy, and radiation can help slow the disease down, they rarely offer a permanent solution.
Recently, however, a new approach using CAR-T immunotherapy has produced some truly astonishing results. In a small US clinical trial, patients with recurrent glioblastoma saw their tumors shrink dramatically mere days after they began treatment.
While it’s still early, this breakthrough has given both the patients facing this form of cancer and the medical community a fresh sense of hope that this deadly disease may one day be treatable.
Understanding glioblastoma
Glioblastoma, often called glioblastoma multiforme or GBM, is the most aggressive and most common malignant brain tumor in adults.
It starts in the glial cells of the brain or spinal cord, whose function is to support and protect our neurons.
When these cells turn cancerous, they start growing incredibly fast and integrate into the surrounding brain tissue.
Unlike most other tumors that form as organized masses, glioblastoma spreads into the nearby areas, which makes it nearly impossible for surgeons to remove it entirely from the body during surgery.
Even in those cases when surgeons believe they managed to remove the tumor completely, microscopic cells are often left behind, which cause the cancer to return again.
While glioblastoma can affect people of any age, it is usually present at older adults. According to the National Cancer Institute, some of the most common symptoms people with glioblastoma experience are persistent headache, seizures, nausea, blurred vision, and issues with their memory and speech.
Because most of this symptoms are common for a number of other neurological conditions, glioblastoma is other diagnoses in its later stages.
The extent of this disease is staggering. As per the charity Brain Tumour Research, about 3,200 people are diagnosed with glioblastoma each year in the UK alone.
Even after decades of research, the sad reality is that the prognosis for patients battling glioblastoma is grim.
The standard “triple threat” of treatment, which involves surgery followed radiation and chemotherapy treatment with drugs such as temozolomide can ease the symptoms and slow things down, but they rarely help get rid of the disease for good.
For patients diagnosed with this type of cancer, the average survival time following diagnosis is usually 15 months, which speaks volumes of the urgency with which researchers and medical professionals should search for new ways to approach the disease for better outcomes.
The challenge of treating solid tumors
What is challenging about glioblastoma is the very nature of solid tumors. While blood cancers travel through the system, a tumor is essentially a clump of cells with its own internal environment.
In fact, even within a tumor of glioblastoma cells, there may be several different kinds of cancer cells with different genetic mutations.
This is called tumor heterogeneity, and it is a major obstacle to treating glioblastoma. It is what makes it so difficult to get rid of all of the cancer cells at once.
It is what makes it so that a treatment may appear to be working at first, only to have the cancer recur later as the resistant cells continue to grow.
The brain itself adds its own layer of defence. While it is wonderful that our brains have this blood-brain barrier that keeps it protected from toxins, it also blocks medications from reaching the tumor cells effectively.
All these challenges have forced experts and researchers from exploring new ways of approaching the processes of treating glioblastoma.
What is CAR-T therapy?
One of the most promising breakthroughs in cancer treatment lately is CAR-T therapy. CAR stands for Chimeric Antigen Receptor T cell therapy, and is essentially a form of personalized immunotherapy that utilizes the power of our own immune system to fight and destroy cancer cells in our body.
The process of CAR-T therapy, according to the American Cancer Society, begins with collecting T cells from the patient or from a suitable donor.
T cells are specific immune cells that identify and fight against harmful invaders in our body. Next, these T cells are sent to the laboratory where they are genetically altered to recognize specific proteins found on the surface of cancer cells.
Once they are re-engineered, the T cells are injected back into the body. When they are in the bloodstream, T cells target their mission and eliminate cancer cells.
So far, CAR-T therapy has shown incredible results in treating blood cancers such as leukemia and lymphoma.
In fact, there have been remarkable examples of patients with leukemia and lymphoma who have run out of treatment options and underwent CAR-T therapy, which led to long-term remission.
However, the difficulty has been in using this this therapy to treat solid cancers, including glioblastoma.
A new approach to CAR-T therapy
Researchers at Mass General Cancer Center, part of Mass General Brigham healthcare system in Boston, have reported promising data on a new CAR-T therapy specifically targeting glioblastoma.
This was reported in March 2024 and has been published in The New England Journal of Medicine, which is considered one of the top medical journals in the world.
According to Mass General Brigham, this study tested a new approach that pairs CAR-T cells with special kinds of antibodies called T-cell-engaging antibody molecules (TEAMs).
This combination has been designed to defeat one of the biggest hurdles in the treatment of glioblastoma, which is the genetic diversity of the tumor. Instead of targeting one specific cancer marker, the therapy has been engineered to target many kinds of tumor cells at the same time.
Dr. Bryan Choi, a neurosurgeon and associate director of the Center for Brain Tumor Immunology and Immunotherapy at Mass General Cancer Center, explained the importance of the therapy.
“The CAR-T platform has revolutionized how we think about treating patients with cancer, but solid tumors like glioblastoma have remained challenging to treat because not all cancer cells are exactly alike and cells within the tumor vary,” Choi said.
Further, Dr. Choi stated that by combining two forms of therapy, researchers are now able to treat glioblastoma in a broader and potentially more effective way.
The first clinical trial involved three patients who had recurring glioblastoma after undergoing conventional treatment, which included surgery, radiation, and chemotherapy.
Each of the patients was given a single infusion of the modified CAR-T cells, and the results were striking.
According to the study published in The New England Journal of Medicine, one patient experienced a tumor reduction of 18.5 percent just two days after receiving the treatment.
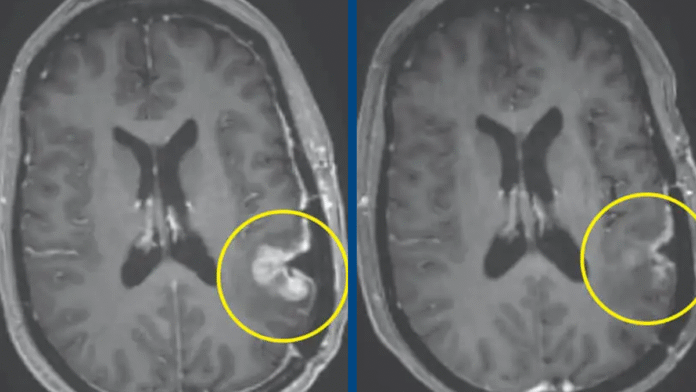
By day 69, imaging scans showed that the tumor had shrunk by 60.7 percent, and the response lasted for more than six months.
Another patient’s tumor was also said to have regressed quickly.
The most impressive case was that of a 57-year-old woman, who, according to Mass General Brigham, had shown near complete regression of her tumor just five days after receiving a single infusion of this therapy, as shown in her MRI scan.
For a disease known for being hard to treat, this is quite rare.
Safety and side effects
However, though the results were encouraging, it is to be noted that there were temporary side effects with the treatment.
According to the researchers, almost all of the patients suffered from fever and temporary neurological symptoms such as confusion or altered mental status shortly after receiving the infusion. Such side effects of CAR-T therapy are common, as the immune system is highly activated to attack cancer cells.
The patients were closely monitored during their stay at the hospital before they were discharged.
Progress but not yet a cure
The results at the three patients whose tumors shrunk have been dubbed remarkable, but still, researchers state that this is not yet considered a cure for glioblastoma.
After some time, the tumors at all three patients started growing again, and according to scientists, this is probably due to the limited presence of T cells inside their bodies.
According to Mass General Brigham, scientists are working on finding a way to make the durability of the treatment more lasting at patients who are battling glioblastoma, including repeated CAR-T infusions or combining the therapy with chemotherapy to strengthen the immune reaction.
Dr. Elizabeth Gerstner, a neuro-oncologist at Massachusetts General Hospital and co-author of the study, highlights the importance of further research despite the progress presented with the recent findings.
“We report a dramatic and rapid response in these three patients,” Gerstner said. “Our work to date shows signs that we are making progress, but there is more to do.”
At the time being, the CAR-T therapy represents one of the most personalized approaches to treating cancer.
By using the body’s own immune cells, scientists are able to create treatments tailored to the specific needs of each individual cancer patient.
Future research may validate these early results, and CAR-T therapy may lead to new avenues of treatment for not only glioblastoma, but many other types of cancer as well.
As Dr. Marcela Maus, director of the Cellular Immunotherapy Program at Mass General Cancer Center, explained in the Mass General Brigham report, the ultimate goal remains ambitious.
“We haven’t cured patients yet, but that is our audacious goal.”
*Medical disclaimer: The information in this article is intended for general informational purposes only. It should not be considered medical advice. The treatment described is still under investigation in clinical trials, and further research is needed before it becomes widely available. Always consult a healthcare professional regarding medical conditions or treatment options.